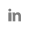
For Melroy Koehler, transplant morning arrived with a surprise: his own bubble parade. He grinned as nurses lined the corridor and blew bubbles—a lighthearted send-off before two, back-to-back, life-changing operations.
“It was special from the very beginning,” said Koehler.
A living donor had given 60 percent of his liver so Koehler could receive the transplant he needed to recover from liver cancer. He was also tipping the scales at 270 pounds, a weight that further threatened his overall health and recovery. So, immediately after his surgical team replaced his diseased liver with a healthy one, they performed a gastric sleeve procedure that removed part of his stomach and reduced his excessive weight. The two surgeries, performed together in just a few transplant centers, took nearly 12 hours and a tremendous amount of surgical experience and skill.
“I dropped weight fast. I was at one point losing between three and six pounds a day and currently I’m about 203 pounds. It helped tremendously in getting back on my feet because I had lost a lot of that weight that was holding me down,” Koehler said.

Expanding Who Can Receive Care
For many patients, the hardest moment isn’t the diagnosis, it is being told there’s no path forward. Koehler’s case is one of many that define University Health Transplant Institute where the medical team pushes the envelope of what’s possible to provide transplants for patients others turn away.
The team is now transplanting candidates with high BMI, fatty-liver disease or colorectal cancers that have spread to the liver. They’re using perfusion technology to extend the life of a liver outside the body until it can be evaluated for use. They’ve also increased the transplantation of DCD organs; those donated after circulatory death. They are historically harder to place, but their effective utilization ensures more patients receive liver transplants when time is of the essence.
“Patients with end-stage liver disease face a terminal diagnosis if they don’t have the option of transplantation,” said Patricia Jones, vice president of organ transplant and donation services. “We recognize that many of our patients come with complex medical, social or behavioral challenges that may have contributed to their illness. Our philosophy is not to judge those circumstances, but to help them overcome barriers and become strong candidates for transplant,” Jones said.
Dr. Tarunjeet Klair, surgical director for the Living Donor Liver Transplant Program, says broader access and stronger results come from rethinking surgery itself. In December 2023, they performed the first combined liver transplant and sleeve gastrectomy for a patient with end stage liver disease who is still thriving today. When chemotherapy or radiation were the traditional treatments for patients like Koehler with liver cancer, the team pushed ahead with the option of transplantation which is greatly extending the patients’ lives.
“I’m proud that we’ve raised the bar and the complexity of the cases we do to a different level,” Dr. Klair says. “The outcomes of both donors and recipients have been excellent.”
A National Model for Liver Transplants
Across the country, few liver transplant programs can match the record set by University Health Transplant Institute, now in its 55th year. The team performed 158 liver transplants in 2024, placing University Health among the nation’s highest-volume centers. For three years in a row, the prestigious INTERLINK managed care organization has named it the No.1 liver transplant center in the United States after examining more than 80 programs. Insurance companies use their findings to determine where transplant patients are likely to have the best recovery.
According to the most recent reporting period of the Scientific Registry of Transplant Recipients (SRTR), one-year patient survival was 97% compared to a national average of 94%, and one-year graft survival with a living donor reached 98%, also higher than the national average.
Those numbers reflect a deep partnership among University Health, UT Health San Antonio, and the Texas Liver Institute—three teams aligning research, education and surgical expertise to give patients the strongest chance at recovery.
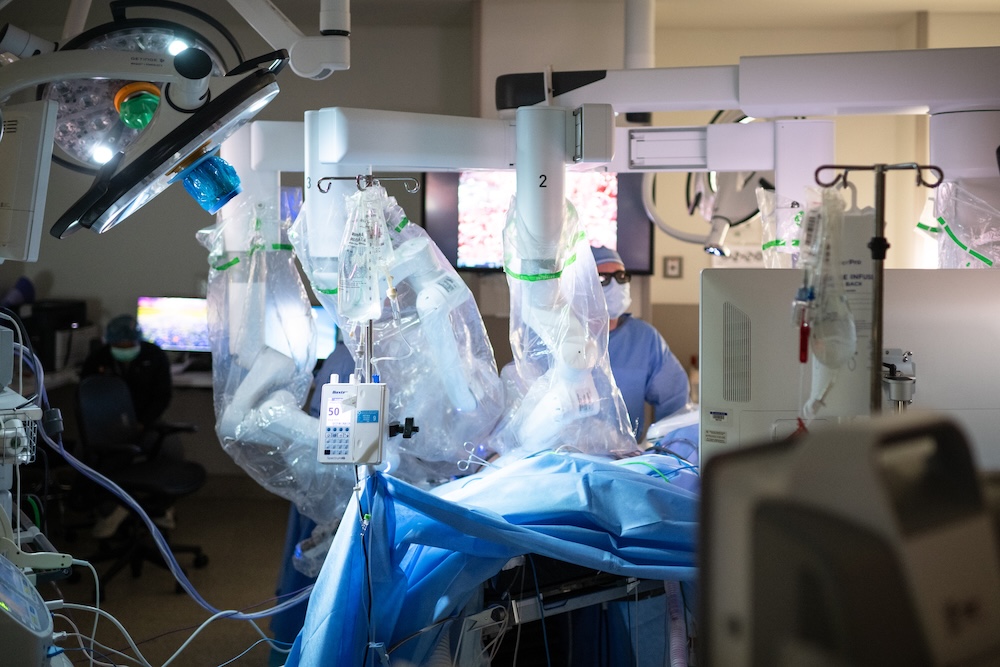
The Power of Living Donation
For people waiting for a liver transplant, time is often the greatest enemy. Living donation can move surgery up by months or more. When a healthy person donates part of their liver, the organ restores itself to full size and function in both donor and recipient. At University Health Transplant Institute, educating the public about the benefits of living donation is central to access and outcomes. In 2024, nearly 42% of adult liver transplants at the Transplant Institute came from living donors—one of the highest rates in the nation—reflecting a sustained push to shorten waits and improve results.
The Transplant Institute expanded the availability of living liver donations by pioneering the nation’s first paired living-donor liver exchange: Two donors incompatible with their intended recipients were matched with other suitable liver patients in exchange for their original recipients also receiving transplants. The program is now able to connect multiple pairs of donors with best-suited recipients, expanding the number of liver transplants and creating model other centers are following.
Champion for Life
Most patients needing a kidney or liver transplants would never dream of asking others to be their organ donors, even though there are an unbelievable number of generous people who are willing to step forward. Knowing that, University Health launched its Champion for Life program in 2020. Its staff educates the public about living donation and helps patients organize a low-pressure search for potential donors. They guide patients in using social media, commercial media and their networks of friends and family to tell their stories. In its first four years, the program helped identify at least 149 living donors. In 2022 alone, it contributed to a 39% rise in kidney donors and a 32% rise in liver donors for the Transplant Institute. The program has since shared its playbook with nearly 30 hospitals nationwide and earned Donate Life America’s 2023 Pinnacle Award for effective organ donation.
Innovation That Cares for Donors, Too
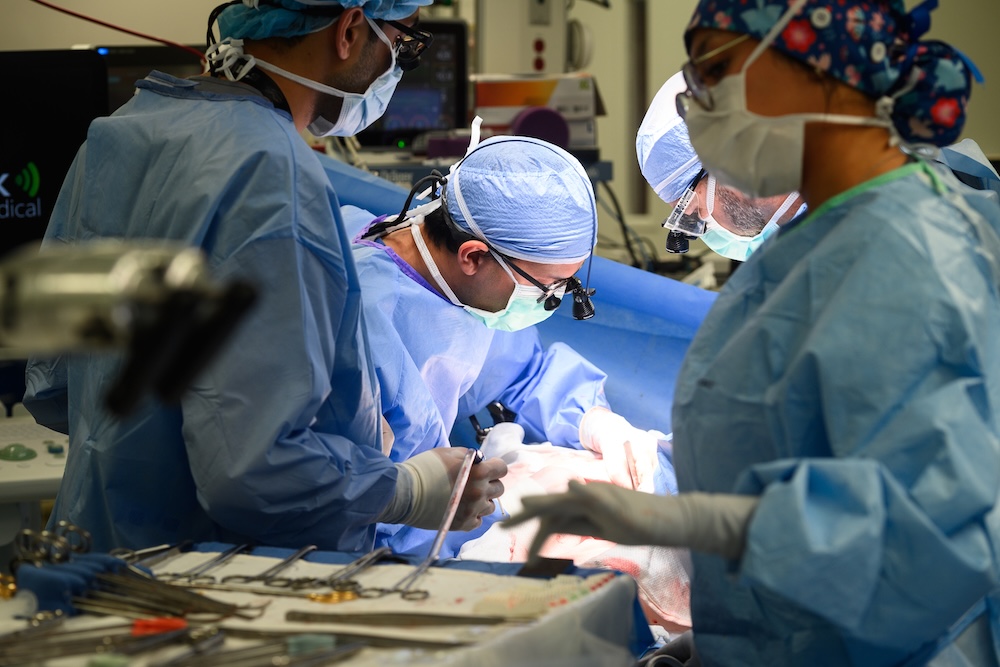
As surgeons expand what’s possible, they’re also reimagining recovery—especially for those who give. University Health is among the few programs performing robotic donor hepatectomy, a minimally invasive approach that removes part of the liver through smaller incisions. According to the Transplant Institute, its broader use of robotic techniques in liver surgery is shortening operation times and reducing the amount of post-transplant medication. Patients are recovering more quickly.
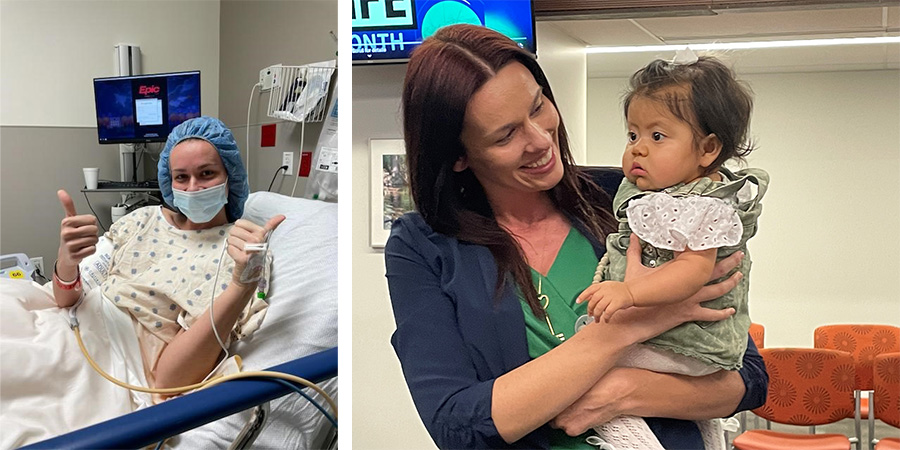
The Next Generation: Pediatric Excellence and Community Support
Children from around Texas and other states often come to University Health when they need a life-saving liver transplant. It has the only living-donor liver transplant program for children in South Texas and one of the few in the country. In 2023, a $1 million gift from the McCombs Foundation strengthened the program and established the McCombs Surgical Director of Pediatric Transplantation, a role held by Dr. Danielle Fritze. Her team’s work continues well beyond surgery, helping young patients learn to manage their care as they grow.
Restoring Health, Sharing Hope
Jennifer Milton, chief administrative officer of transplant, says the real measure of success is what happens after patients receive their new organs.
“When we measure outcomes, these people are going back to work quickly,” she says. “They’re going back stronger—not just medically, but well and whole to their family. We’re seeing whole, well families and communities again because we’ve said ‘yes.’”
The team’s expertise now reaches far beyond San Antonio. Dozens of hospitals across the country have adopted University Health’s protocols for living-donor and donor-care programs.
For patients like Melroy Koehler, that commitment to push the boundaries of traditional transplant care means everything. He is cancer-free, off diabetes medications and living life with a healthy weight.
“Every individual—the nurses, the doctors, even the people who brought my food—they all saved my life,” he said, adding, “It’s good to be alive.”
Learn more about liver transplantation, living donation, and the Champion for Life program at UniversityHealth.com.
Reference: https://storystudio.expressnews.com/2025/11/14/the-hospital-that-says-yes-inside-the-nations-top-ranked-liver-transplant-institute/